BY GAMUCHIRAI MASIYIWA
Summary: Zambia is as generous with patients from neighboring Zimbabwe as it is with its own citizens. That could mean problems for both countries.
This story was originally published by Global Press Journal.
MASHONALAND WEST, ZIMBABWE — When Dube was diagnosed with gallstones in 2013, the public hospital in Zimbabwe recommended surgery costing close to 4,000 United States dollars. She couldn’t afford that.
A friend suggested she go to Zambia, about 150 kilometers (94 miles) to the north. There, the friend said, treatment would be cheaper.
Over the past decade, Dube has gone to Zambia multiple times for medical treatment. Her most recent trip was in June. Treatment is cheaper there, she says, but the level of care is also far better than what she would get at home. Dube asked that Global Press Journal use her totem name, a symbolic representation of ancestral lineage, out of concern about Zimbabwe’s Patriotic Bill, which discourages criticism of the government.
In the 1980s, Zimbabwe had one of the best health care systems in sub-Saharan Africa. But over the years, this glory has faded. An ongoing economic crisis spanning over two decades has left the health care system scrambling to meet the needs of its population. Skilled health care workers have left in droves, drawn to opportunities abroad. More than 4,000 health care workers left Zimbabwe in 2021 and 2022 alone, according to government statistics. By late 2022, Zimbabwe had about 1,700 doctors and about 17,200 nurses to serve a population of 15 million people.
Just as health care workers are leaving the country, so are patients.
Over the past decade, Zimbabweans have spent more than 4 billion US dollars on cross-border medical migration. Annually, more than 200,000 Zimbabweans spend around 400 million US dollars on specialized medical treatment abroad. India, China, Singapore and South Africa are the main destinations.
But an increasingly popular choice is neighboring Zambia. In April alone, the International Organization for Migration surveyed over 260 people migrating from Zimbabwe to Zambia. When asked why they were traveling, 42% stated that it was to access better services — health being the top priority.
Precise data is hard to come by, but anecdotal evidence from sources who spoke to Global Press Journal, including border officials, points to a growing trend, raising questions about Zambia’s ability to manage the influx, and the future of health care in Zimbabwe.
The choice of Zambia
Zambia and Zimbabwe allocated nearly the same amount of money to their health sectors in 2024, even though Zambia is home to 4 million more people. With that budget, it’s an unlikely alternative to the Zimbabwean healthcare system. And in Africa, it’s South Africa and Kenya that are top destinations for medical tourism.
But the border with Zambia isn’t far for many Zimbabweans, making the cost of travel low and the process of crossing the border usually straightforward. A person needs either a passport or a pass issued at the border for just 1 US dollar, says Morgen Moyo, assistant regional immigration officer at the Chirunduborder post.
Even without documentation, immigration officials will at times let those seeking health care pass through. “Zambians prioritize life,” Moyo says.
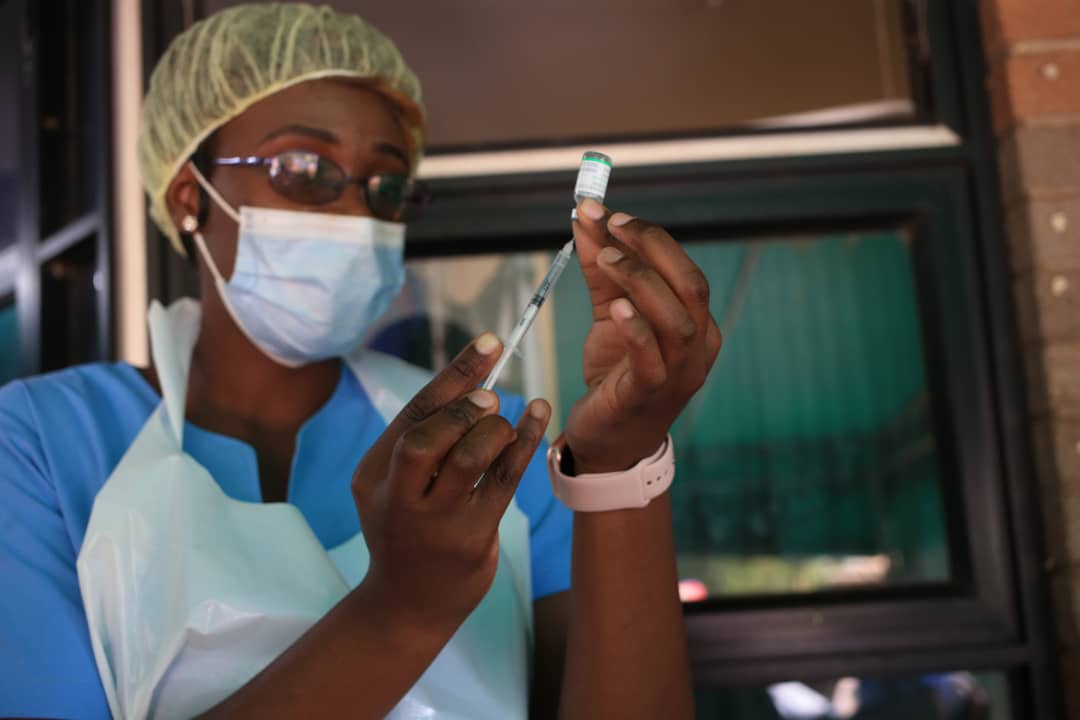
It’s not only about convenience. Zambia offers free primary health services, including basic treatment, preventative care, vaccinations and maternal health care services, according to the 2022-2026 Zambia National Health Strategic Plan.
While these free services are not available to foreigners long-term, they can access them in emergencies within the first 24 to 48 hours in the country, says Dr. Kennedy Lishimpi, permanent secretary of administration for the Zambian Ministry of Health. Foreigners are expected to pay for Zambian health care after that timeframe.
In practice, though, Zambian health workers rarely charge foreigners, according to a 2019 study paid for by the US Agency for International Development, known as USAID.
“You wouldn’t want to see somebody from Zimbabwe, for instance, getting to Zambia and not accessing a service and then they end up dying. That is not good. Similarly, we expect that our sister countries do the same to our citizens when they are there,” Lishimpi says.
Dr. Mwanza, a Zambian doctor who chose to use only his last name for fear of retribution, says availability of surgical and specialist services in Zambia drives medical migration. In Zimbabwe, these services are rarely available outside of the large provincial and central hospitals. In 2019, for example, about 10% of district hospitals could provide basic surgeries, compared to 83% of provincial and central hospitals, according to a Zimbabwe health ministry assessment.
When Mary Chipfuvamiti’s son broke his arm in June, she says she chose a hospital in Zambia — about 93 kilometers (nearly 58 miles) from her home — over local options. She suspected the local hospital’s X-ray machine wouldn’t be working, and they would likely refer her to a private facility where an X-ray would cost her 40 US dollars.
“I only had 30 dollars on me,” she says. In Zambia, the total cost came to about 12.50 US dollars.
A case for Zimbabwe
Things haven’t always been like this in Zimbabwe. Before the country’s economy took a downturn, it offered free health services in the 1980s to low-income earners. About 90% of the population fell in that bracket.
In the early 1990s, the government introduced user fees in public health facilities as part of the austerity measures imposed on the government by the International Monetary Fund to reduce government expenditures. Currently, free health services are offered only to pregnant and lactating mothers, children under age 5 and adults over 60.
The economic crisis continues to strain what remains of the health care system. Hospitals struggle with obsolete infrastructure. Shortages of medicines and supplies in public health facilities are the norm.
And although Zimbabwe and Zambia have similar health budgets, Zimbabwe’s treasury sometimes delays funds disbursement, says Norman Matara, secretary general for the Zimbabwe Association of Doctors for Human Rights.
That was the case in 2021, when the health ministry by September had used just 46% of its budget allocation for the fiscal year due to late disbursement of funds, according to a 2024 situational report by the Zimbabwe Coalition on Debt and Development, a nongovernmental organization that advocates for socioeconomic justice.
“There is a mismatch between the money that is put on the budget and what is being received by the health institutions,” Matara says. Reasons include hyperinflation and currency rate fluctuations, he adds.
Comparing health services across countries is unfair, says Donald Mujiri, a Zimbabwe health ministry spokesperson. “Each country has its set standards and pricing.”
He doesn’t think this migration of patients reflects poorly on Zimbabwe’s health care system. “We have all the services in the country, and they are adequate to serve the people,” he says, adding that people are free to seek health care where they want.
Mujiri did not address questions regarding the late disbursement of funds.
The cost of the journey
These journeys to Zambia come with challenges.
Dube recalled her trips along the bumpy Harare-ChirunduHighway that connects the two countries, when every bump caused piercing pain.
In 2019, six years after her initial treatment in Zambia, she began experiencing severe pain. She went to a hospital in Harare for treatment, but a few months later the pain resurfaced. By that time, there was a health care strike at home, forcing her back to Zambia for treatment. Then in 2023, Zambian doctors discovered metal clips from her earlier surgery in Zimbabwe were piercing her liver. She returned to Zambia in January this year for corrective surgery, and again in June.
Health care experts warn that such journeys can be especially risky for patients who undergo surgery. If a surgery is performed in Zambia and there is no proper follow-up, there can be complications if doctors in Zimbabwe are unaware of previous procedures or tests, says Mukanya, a health expert working in a Zimbabwean hospital who chose to use his totem, fearing that speaking to the media would cost him his job.
In the case of misdiagnosis or malpractice in a foreign country, it’s difficult to get recourse. “In most cases you are powerless because you don’t know the [reporting] process and approaching a lawyer may require money,” he says.
Medical migration also comes at a cost to Zambia. The influx of patients complicates health planning, leading to shortages of essential medications and making it difficult to allocate resources effectively, according to USAID. The agency’s report recommends the Zambian government create a fee-for-service system to discourage foreigners from seeking free health care, but doctors in Zambia don’t seem to agree.
“Most health care providers interviewed stated that they would continue to provide services free of charge should a foreign patient be unable to pay,” according to the USAID report.
Lishimpi, the Zambia health ministry official, had no comment on the report’s concerns.
Dube, who is recuperating at home, is uncertain about the solutions. But she thinks the Zimbabwean government needs to prioritize fixing her country’s health care system. “I don’t know how best we can help our hospitals, but if there was any other way, I think they should consider the health sector more than anything else because we are talking of human life,” she says.
Gamuchirai Masiyiwa is a Global Press Journal reporter based in Harare, Zimbabwe.
Global Press is an award-winning international news publication with more than 40 independent news bureaus across Africa, Asia and Latin America.


 Slider3 years ago
Slider3 years ago
 National5 years ago
National5 years ago
 Tourism and Environment4 years ago
Tourism and Environment4 years ago
 Special reports4 years ago
Special reports4 years ago
 Opinion4 years ago
Opinion4 years ago
 National4 years ago
National4 years ago
 National3 years ago
National3 years ago
 National3 years ago
National3 years ago